It’s September and that means one thing – CMT Awareness Month. During the month of September I will be using my blog to play a part in raising Awareness with an “alphabet challenge” – blogging a letter / key word almost every day. Today is brought to you by the letter Q. I hope my blogging will help you to learn more about CMT – the most common but least well known hereditary nerve disorder – and me. And I hope this will also help to raise funds for the Charcot Marie Tooth Association to support its efforts to find a treatment for CMT. You can join me in learning more about CMT by clicking onto www.cmtausa.org and of course a donation would be wonderful too!

I thought I’d change today up and see if anyone had any questions about living with CMT for me. Here are a few.
1. How did they diagnosis your hypermobility in addition to CMT?
The question continues…
“I’ve asked and heard that my “loose joints” are a part of having CMT. When does CMT end and a co-condition begin?”
I received my diagnosis of CMT in 2004 after walking a half marathon and having a very angry left foot. My weak peroneal muscles had led to inflammation in the spot where the peroneal tendon inserts into the foot bone — too much ankle roll while walking triggered a lot of pain and swelling.
I was diagnosed with EDS-3 (hypermobility type) in 2007 after rotationally dislocating my elbow. The orthopaedic surgeon performed a simple Beighton test.
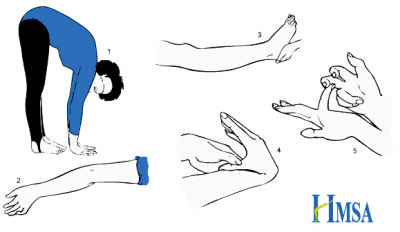
More on the Beighton score from the Hypermobility Syndromes Association.
Back in 2007 I was still doing yoga three times a week, so I was a 9/9 on the scale. Nowadays, with less yoga and more cycling, plus a reconstructed elbow, I am 5/9 on the scale.
A Beighton score is only the first step in a diagnosis though. Hypermobility Ehlers Danlos is caused by defective collagen protein structures in connective tissues. There are other physical manifestations – very easy bruising (and often bruising appears for no apparent reason). Very stretchy skin. Scars healing with wide scar tissues (kind of like keloids). Very low blood pressure or erratic changes in pulse. Heat regulation issues. Joint pain.
With CMT, a lot of joint instability is a result of having poor nerves leading to muscle atrophy – so the muscles cannot stabilise the joints well. We often can have loose ankles (which in turn get looser the more regularly we turn them) and loose knees. But hypermobile joints are different. It is a connective tissue problem – not muscle related instability.
A good rheumatologist or orthopaedic specialist can help to make a diagnosis.
In the meantime, here’s an interesting article on hypermobility versus flexibility. And yes – I am hypermobile and lack flexibility – especially in my tight CMT legs!
2. How does having a puppy help (or not) with CMT?
It is no secret that in January we got a puppy. Felix 3Spot has been a complete game changer in our lives.
You can kind of see that I am wearing my Got Nerve for CMT Awareness Month t-shirt!
My neurophysio said it to me best:
“Having a dog will make you naturally work on and improve your stabilising muscles which have a tendency to atrophy due to CMT.”
I find this aspect also the most challenging. When Felix tugs it is hard for me to stay stable. It is why getting a good harness solution has been so vital and has made our walks so much more pleasant – less tugging (and instability for me!) with a front clasping harness!
The good thing about Felix is that he needs activity. He is a super active dog breed, so needs walks – mornings, evenings, and in betweens. So there is no excuse to just sit at home on the sofa. And that means that – for good or bad, when I am fatigued or not – I am out making sure he is active. As activity is the best and only medicine for CMT this is a huge benefit for me too.
I think on balance having a pet is a great idea for people with chronic conditions who would benefit from physical activity.
3. I’ve seen quite a few online posts about people with CMT having below the knee amputations. Why do people opt for amputation? Is it because the nerves die? Is amputation a certainty for everyone with CMT?
A path to wheelchair use, ankle foot braces, or amputation is not set in stone for those of us with CMT. CMT is a progressive degenerative disorder that impacts each individual differently. So there is no certain path – except for the path that we should expect declining over time.
Amputation is an option for ANYONE with chronic issues involving foot pain, surgeries gone wrong, breaks that won’t heal – as well as CMT.
I am aware that amputation can seem an extreme solution – but what most amputees find is that with the removal of the chronic limb problems they have a radically improved quality of life. I have found this to be the case in the people I have met who have opted for amputations following cycling accidents, being hit by cars, and as a way to manage the way CMT impacts their life.
Doctors will always try to help to find a solution. And surgery is one option for people trying to manage chronic foot drop (the inability to lift your feet up while walking). But sometimes surgery does not work, or needs to be repeated. It is not unusual to hear of people having more than 10 surgeries per foot to try to find a solution to problems caused by CMT. I can completely understand that after so many surgeries and things going wrong that a logical next step could be amputation.
Anyone opting for a voluntary amputation goes through a complete psychological screening to make sure they are a good candidate for the procedure. Let’s face it – life without a part of a limb is life altering, and you need to be in a good place to be able to make the necessary adjustments. A good place to not only deal with the immediate change – but also to deal with the knowledge that you still need to work hard to adjust, adapt, and find solutions. It can take a long time to get things right. Just like it took me seven years of working with an orthotist to get the right shoe inserts, it can take an amputee just as long to work with a prosthetist to get the right socket fit for a prosthetic limb.
So is amputation because nerves die? Perhaps – if neurological pain is localised to the feet and a doctor and patient agree could be best managed through amputation. But in general, it is not the problem with the nerves that causes the amputation. It is the consequence of nerve problems – the muscle atrophy, foot drop, foot contracture due to loss of small muscles in the feet – that leads one to consider surgery and eventually amputation.
Not such a simple question!
4. How do you deal with the fact that CMT is progressive and degenerative?
I guess the question is about dealing with uncertainty.
To be perfectly honest when I got my CMT diagnosis I did two things. First I googled and saw that my future may involve a wheelchair. This made me want to ignore my diagnosis. So as a response to that I did the second thing – I joined a Yahoogroup for people with CMT to learn as much as I could about the disease.
Over time I have gone through swings and roundabouts when it comes to managing life with CMT. I ignored it for a while – in fact, I ignored healthy living in general for a good few years. That was a mistake, and in 2009 I decided to make a change and embrace triathlon and healthy living as a way to manage my CMT.
In more recent years I have learned that for me, I have to learn my limits and test them bit by bit to feel at ease with my body, with myself, with what I feel comfortable doing and taking on. I once had a goal to do an iron distance race by 2015. As recently as 2013 I thought this might still be a possible goal for me. But throughout 2013 and 2014, I have done a lot of self reflection and soul searching. And decided that what makes me happy is not having huge goals like an ironman, but achievable goals that represent my own personal ironman (regardless of distance or race).
Ironically it is not CMT that I think about when setting my goals and physical challenges (as I do believe with my current state of CMT it is not a true limiter) – rather it is my other chronic condition EDS!
Now, as far as managing through uncertainty. There are some key things triathlon has taught to me. First on the list is that I can only control what I do today. So that is what I do – I focus on each day, as it comes.
So when I set my physical goals, I work with my coach to have a daily plan to take me to the best physical place to achieve that goal. I work on being flexible enough mentally to know that if on a given day I am just not able to do the work (like right now, for example: I haven’t trained in three days due to a jaw injury Sunday evening and a horrible sore throat) I draw a line under my non-performance and move on. Focusing on the next day. And what I CAN DO now.
For me, it is all about being here now. Not an uncertain downward slide. But the positives of today.

This also kind of relate to something Kim Ingleby said at a mental strength workshop she hosted. She said that if we are motivated by fear, that we will not succeed as individuals.
When I first started living with my diagnosis of CMT, I was motivated by fear. I did not want to decline. I was scared of a future with less mobility. I sought answers and acted in ways to “manage my condition” – to prolong my date of decline. Out of fear. But deep down this made me SO UNHAPPY. So I made a choice. After that workshop in April 2011, instead of running away from CMT and being mad at my body and my genes for dealing me this hand of cards, I decided to stop fighting myself and to just focus on what I COULD do and how I COULD do more. I ran toward my goals, rather than away from my fears. I decided to make CMT my friend, working to understand my body in order to work with my body – instead of always pushing myself and punishing myself for what I could not do. 2011 was my breakthrough year – the year I realized I could achieve more than I had ever dreamed.
Be here now. Dream big dreams – and act on those dreams today, taking small achievable yet stretching steps to turn those dreams into reality.
It’s CMT Awareness Month. Today’s post was brought to you by the letter “Q” – questions. You can learn more about CMT and donate to support the search for a treatment for this (at present) incurable progressive degenerative nerve disease at www.cmtausa.org — Thank you!
